This was not a planned topic. This is a topic about a journey that I have been on for three months now (since May 2021).
As time went on in my journey, with the more things that started going wrong for me I decided that just like our grief journey, needed to be shared. It needed to be shared to bring further awareness of this condition, and to help to make people aware of the complications that can occur due to this condition…..
Please see My experience of Pilonidal Cyst/Abscess Surgery: Staphylococcus Aureus bacteria/Sepsis (early stages):
- Introduction
- Pilonidal Disease
- Pilonidal Surgery
- Pilonidal Forums/Living with Pilonidal Disease
- Stress and Wound Healing/Taking care of your mental health
- Staphylococcus Aureus bacteria/Septicaemia and Endocarditis
- Peri wound Management
- Peeling Skin
- Our Final Thoughts/Our YouTube Video
© Copyright 2019 Grief Probate Journey Blog *PLEASE NOTE THIS INFORMATION IS SOURCED FROM UK and AMERICAN WEBSITES* It is also based on our own experience. *We are not experts in this field, we are speaking purely on our own experience with information sought from the internet to give further examples. *
1. Introduction
This was not a planned topic. This is a topic about a journey that I have been on for three months now (since May 2021).
As time went on in my journey, with the more things that started going wrong for me I decided that just like our grief journey, needed to be shared. It needed to be shared to bring further awareness of this condition and to help to make people aware of the complications that can occur due to this condition.
My original journey started in May 2012. I noticed a slight pain in my tailbone whenever I was sitting down. This pain got to the point that sitting down was becoming too painful and so I made an appointment to see the doctor. It was confirmed that I had a pilonidal cyst, it was decided it would be removed by a planned surgical procedure.
I had the procedure which requires the wound to be left open for healing. This means it had to be packed daily so that the wound can heal from the bottom up.
Thankfully for me, my wound was extremely small, and so it was only packed one day after surgery. I couldn’t have been happier because it was so painful getting it packed, it made my eyes water. I can still remember the pain that I felt then 9 years later.
After the wound closed, I did have an incident where the wound had started leaking, I went back to the doctor, but I can’t remember what happened. I know I didn’t require any further surgery.
Over the years, I would get a twinge of pain in my tailbone and sitting would be slightly painful. This would last for maybe a week or so. I googled these symptoms, and it did say it is common to get pains from the wound area, without it flaring up into another cyst. Because of this, whenever the pain came, I just got on with it until it went away again.
Fast forward to May 2021. The pain came, but this pain was different, right away I knew something was wrong, and so I phoned the doctor. I was given antibiotics to take (7 days), however unfortunately it went from me feeling a small lump, to it getting bigger and bigger. Sitting and standing was excruciatingly painful, I was putting all the pressure in my hands and arms to be able to sit and stand.
I could tell the antibiotics were not working, and so I knew I would have to call the doctor to tell them before the course ran out.
I didn’t get the chance to do this, as it went from being excruciatingly painful to sit down, to not being able to sit down at all. It had turned from a cyst to an abscess. The pain was unbearable, nothing like I had ever felt before.
I called 111, explained my situation and was advised that I need to go to a hospital, I needed to go the same day I phoned because it would be a problem if it burst. I requested which hospital I wanted to go to. I specifically did not go to the hospital which our Dad was an inpatient.
I went that same evening but was not able to have the surgery that night. I was given the option to go home and come back in the morning, but with the level of pain I was in that wasn’t even a consideration. I was admitted overnight, scheduled for surgery the next morning. I was told there was a chance the abscess might burst during the night, but even if this happened, I would still require surgery.
During the night sure enough the abscess burst, this did not decrease my level of pain, and it was confirmed that I would still require surgery to remove the remainder as it had only burst at surface level.
The surgery was over so quickly that I didn’t even realise I had it. When I woke up in recovery, I thought I was still waiting to go into the theatre.
That same day I was discharged to go home. This is when my new journey began. My journey of recovery (We also have a topic on: Triggers Anxiety and Grief which goes into some detail of my hospital experience).
This consisted of Daily dressing changes for 8 weeks. This was my 6th operation, and I have had surgery for this before, but nothing could prepare me for the pain I went through. Mentally and physically this really took its toll on me.
- Everything I did had to revolve around my dressing changes
- I couldn’t make any plans unless I had my appointments set up
- I wasn’t able to drive or do anything strenuous
- I felt helpless to a point.
- I felt like I was in a new lockdown all on my own
The pain was so intense that after dressing changes, I had to come back and rest.
It felt soul-destroying knowing that no matter how tired I was, or how much I didn’t want to go through the pain again, I had to go, if I didn’t, that could be an infection, taking longer to heal. And as I didn’t want any of that, I had to endure it.
I felt like I was living through Groundhog Day. I felt like I was continuously on antibiotics back-to-back. The routine of the antibiotics dictated as and when I ate, it all started becoming too much, I just felt like there was no end in sight.
The wound got infected twice.
The second time it got infected it went into my bloodstream and I was in the early stages of sepsis. I was so ill, this drained all of me in less than 24 hours. It was such a scary experience as everything developed so quickly, and before going for my daily dressing change where it was confirmed, I had no idea why I had suddenly become so ill so rapidly.
(We also have topics on Sepsis, Sepsis Awareness, World Sepsis Day 13th September 2020, Guest Blog: Rachel and Dave telling their Sepsis Story: Scoot for Sepsis Campaign).
Before treatment for this infection:
- A rash developed on the top half of my body
- My body was itching internally all over
- I was feeling as though I was going to throw up and pass out at the same time
- I could see green in front of my eyes
- I had a temperature but didn’t realise (my nurse said I was so hot she felt like she was standing next to her oven)
- My hands were red and swollen and painful (mainly my left hand)
- My body was extremely achy
- Any form of movement felt impossible
- My body felt like it weighed a tonne.
After treatment:
The bacetria went into my mouth and on my tongue. This was a difficult time because anything that was hot (spice including my toothpaste) I could not have it on my tongue because it burned. I was so happy when my tongue was back to normal.
The skin on my hands started peeling – the entirety of the skin of my hands peeled off. This took about four weeks. The after-effects of the peeling are my hands, and fingertips are sore. (The doctor has said this is because my nerve endings are exposed until my hands are fully healed).
My feet were swollen beyond belief. I found it difficult to find shoes to wear because of this.
Three weeks after the infection went into my bloodstream, the skin on my feet started peeling.
The skin peeling occurred because of the toxins that the bacteria leaked into my system. The bacteria I was infected with (the second time around) was: Staphylococcus Aureus and Mixed Anaerobic. (When our Dad was an inpatient in the hospital he also contracted a Staph infection, this occured due to the burns on his feet).
Through doing research as I was struggling to find out how long I could be recovering for, how others who go through this feel, and what else I could expect I discovered this bacteria can not only cause septicaemia it also can lead to Endocarditis. This really freaked me out. Our Dad was diagnosed with Infective Endocarditis when he was admitted into the hospital in September 2016 he also contracted Sepis whilst an inpatient in the hospital, but we didnt find this out until after he passed away. For me to know I could contract not one, but two life-threatening conditions, I felt lost for words. (We have topics on Infective Endocarditis and Infective Endocarditis and Blindness).
The reason why I am doing this as a topic as this appears to be a rare known condition,
It is classed as minor surgery
BUT
I never ever expected I would get an infection that would go into my bloodstream causing me to suffer from a life-threatening condition from something that is classed as minor surgery.
The more things that happened to me on my journey, this is when I decided this needed to be shared. It does feel a bit out of my comfort zone, but this is what we do in our blog, we try our best to spread awareness of matters that might not be well known, this is why I felt it is important.
If this topic could help people become more aware of this, and also possibly help someone who is going through it, I would be very pleased.
This felt like a very lonely journey, mentally it really brought me down, physically it also brought me down. I felt like when will this be over, when will I experience normality again. I completely forgot what normality was.
One thing I will say, I am unduely grateful to the nurses doing my dressing changes, my friends and family who supported me through this trying time, and continue to support me. I wouldn’t have been able to make it through without the love, care, and support. The difference it made to me is hard to put into words. I was in a very low place on a daily basis, but the love and support truly helped me to get up every day and keep going. I am thankful, I am grateful, and I am blessed.
I am speaking in past tense as though my healing journey is over, it is not over, my feet are still peeling. In total, I have been going through this for three months now. It has been nine weeks since the infection went into my bloodstream.
In this topic, the links provided are things that I searched for in trying to better understand what was happening to me, and the reasons why. I hope this makes sense in the way I have put it together.
Please see: My experience of Pilonidal Cyst/Abscess Surgery: Staphylococcus Aureus bacteria/Sepsis (early stages)
2. Pilonidal Disease
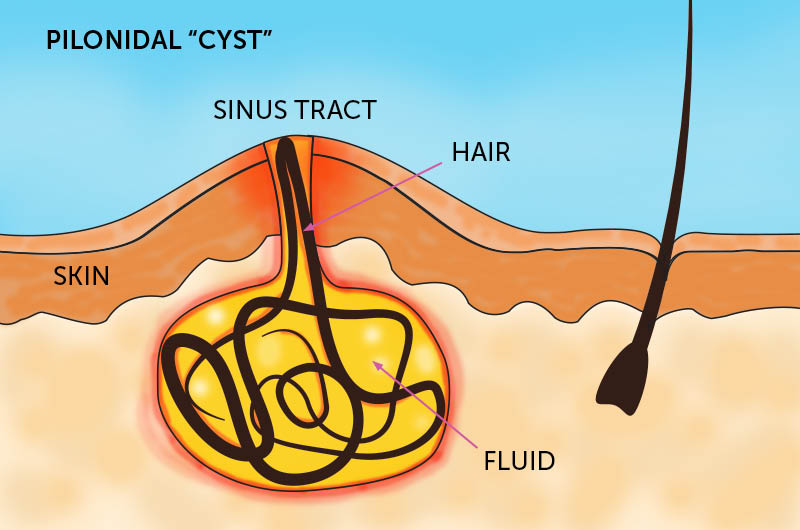
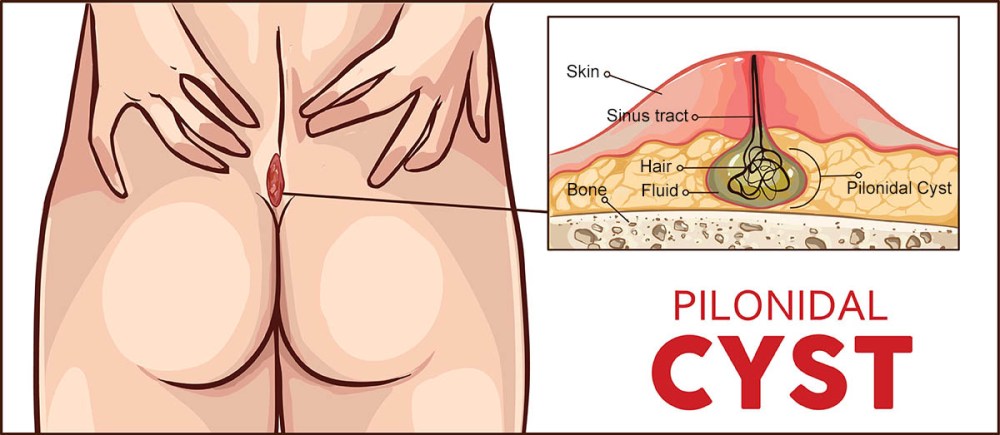
“Pilonidal disease is a chronic skin infection that develops in the crease between the buttocks, near the tailbone”.
2.2 What is Pilonidal Disease?
“Pilonidal disease is a chronic infection of the skin in the area between the buttocks. Pilonidal, pronounced pie-luh-NIE-dul, occurs when hair follicles become plugged. It is a common condition that can happen to anyone but is most prevalent among teenagers and young adults”.
2.3 What is Pilonidal Disease and Ways to Treat it Naturally
“Pilonidal disease is a painful, chronic skin condition in which an individual suffers from frequent pilonidal cysts. These cysts form in the natal cleft near the tailbone. Pilonidal cysts are filled with pus and hair follicles. They can grow to be very large and have the possibility of becoming debilitating”.
3. Pilonidal Surgery
3.1 Surgery to treat a pilonidal sinus – Guy’s and St Thomas’ NHS (SINCE PUBLISHING THIS TOPIC, THIS LINK IS NO LONGER AVAILABLE. APOLOGIES)
“However, surgery is often the only way to treat the cause of the abscess, and remove all the infected tissue. This is also called an excision. Your doctor has”…
3.2 Pilonidal Sinus Surgery MaineHealth
“(24 Dec 2016) — www.mainemedicalpartners.org. Post-Operative Instructions. Pilonidal Sinus Surgery. Comfort Measures: Pilonidal sinus surgery is not” …
3.3 Pilonidal sinus: healing rates, pain and embarrassment levels – PubMed
“by A Stewart · 2008 · Cited by 11 — Pilonidal sinus: healing rates, pain and embarrassment levels. J Wound Care. 2008 Nov;17(11):468-70, 472, 474. doi:”
4. Pilonidal Forums/Living with Pilonidal Disease
4.1 Pilonidal Discussions – UK Forum | Pilonidal Support Forums
“10 Jan 2021 — Discussion on UK specific topics – NHS, Surgeons, etc.. Please post basic Pilonidal questions in the General forum above”. (No images in this forum).
4.2 Pilonidal Care Program | Frequently Asked Questions | Boston Children’s Hospital
“The Pilonidal Care Program at Boston Children’s Hospital specializes in the treatment of pilonidal cysts. Our team has a broad range of expertise in”..
4.3 Living with it – Pilonidal Support Alliance
“(3 Jan 2019) — Living With Pilonidal Disease. Once you know you have a Pilonidal abscess you have two choices: surgery or try to live with it”.
4.4 The moment my life changed. And taking risks suddenly…
“(21 May 2013) — I took a look at the corresponding place on my body, close to my tailbone, and found a small pit. My condition was called a Pilonidal Cyst. I’ll” …
4.5 Reducing the recurrence of Pilonidal Sinus Disease
“(21 Jun 2013 — Primary treatment for PSD is by surgery but there is a high recurrence rate. Laser hair removal reduces the rate of recurrence by diminishing”..
4.6 What You Need to Know About Pilonidal Cysts
“(15 Jan 2021) — Patient education is essential to the success of a pilonidal cyst care plan. … What You Need to Know About Pilonidal Cysts”.
5. Stress and Wound Healing/Taking care of your mental health
I googled these links because of how I was feeling within myself. But what I didn’t realise was how apparent it was to others. I am so thankful to have had such caring nurses that really listened to my concerns and took action when I said I felt something was wrong.
I was seen by 6 nurses over the 8 weeks. Each was so helpful to me in their understanding. Something that they would often say is I have to try and keep my spirits up, be positive and know this is temporary and the wound will heal. They always often said that if I’m sad and depressed it will cause the healing process to slow down.
5.1 Psychological Stress and Wound Healing in Humans: What We Know
“Stress and Wound Healing … It is well established that psychological stress modulates immune system functioning and a fully functioning immune system is” …
5.2 Researchers Learn How Stress Slows Wound Healing
“Scientists investigating why wounds heal more slowly on patients who are stressed have found that psychological stress can increase the levels of some hormones in the blood. These hormones can slow the delivery of certain compounds — cytokines — to the site of the injury to start the healing process”. (28 Jul 1999).
“Depression and anxiety, both, can impair patient’s quality of life (QoL), especially when chronic diseases appear. Chronic wounds are defined as loss of skin integrity with 1 or more underlying structures and absent healing within 8 weeks”. (21 Nov 2017).
5.4 Wound-related Pain: anxiety, stress and wound healing
“by KY Woo · Cited by 55 — Canada. Pain is a common problem in patients with chronic wounds. This article discusses a systematised approach to address and manage wound”–
5.5 Stress and pain associated with dressing change in patients with chronic wounds – PubMed
“by D Upton · 2012 · Cited by 63 — Objective: To assess pain and stress experienced by patients with chronic wounds at dressing change and to examine how this may be related to”…
6. Staphylococcus Aureus Infections/Septicaemia and Endocarditis
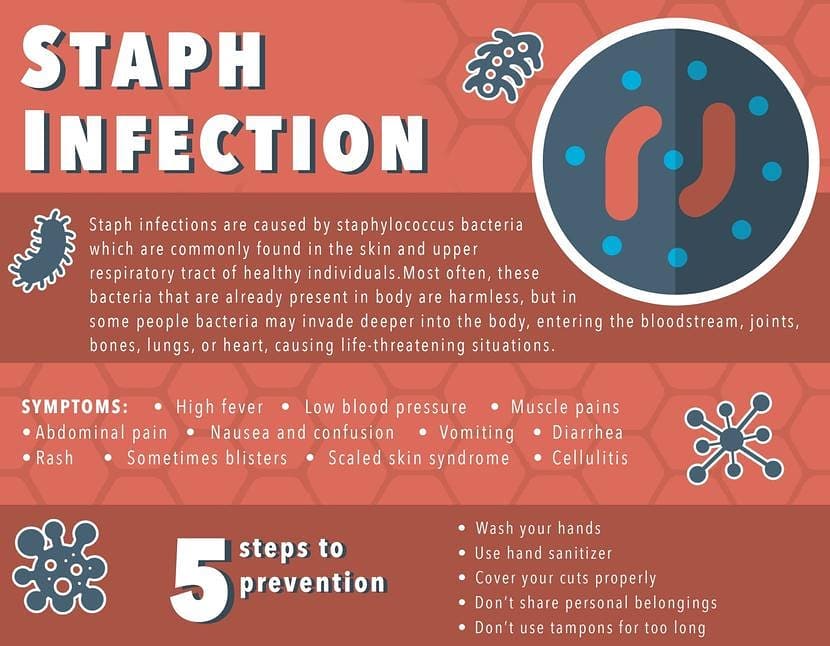
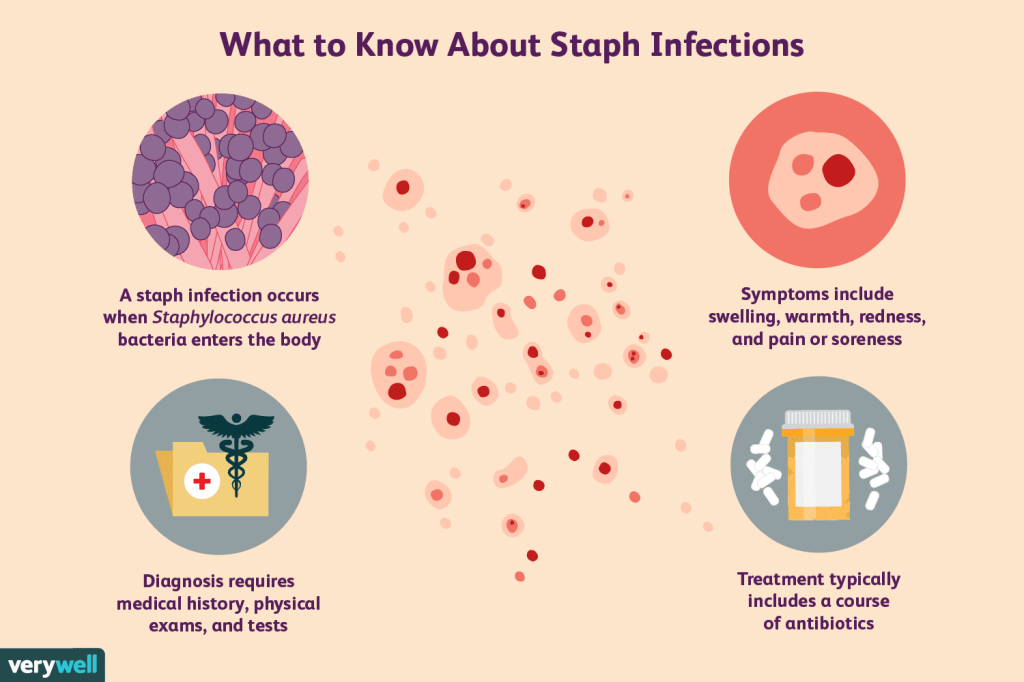
“The bacteria that cause staph infections live harmlessly on many people’s skin, often in the nose and armpits and on the buttocks. They usually only cause an infection if they get into the skin – for example, through a bite or cut. Staph bacteria can spread to others through: close skin contact”.
6.2 Anaerobic bacteria in Septicaemia and Endocarditis – PubMed
“Most cases of anaerobic endocarditis are caused by anaerobic cocci, Propionibacterium acnes and B. fragilis. Predisposing factors and signs and symptoms of endocarditis caused by anaerobic bacteria are similar to those seen in endocarditis with facultative anaerobic bacteria with the following exceptions”.
6.3 Staphylococcus Aureus Infections
“Staphylococcus aureus is the most dangerous of all of the many common staphylococcal bacteria. These gram-positive, sphere-shaped (coccal) bacteria (see figure How Bacteria Shape Up) often cause skin infections but can cause pneumonia, heart valve infections, and bone infections”.
(I DID NOT LINK TO THIS ARTICLE AS IT HAS IMAGES)
6.4 Banish Infection With These 5 Powerful All- Natural Antibiotics
“(5 Apr 2018) — Banish Infection With These 5 Powerful All–Natural Antibiotics · 1.) Oregano oil · 2.) Manuka honey · 3.) Garlic · 4.) Onions · 5.) Echinacea · Bonus: …
6.5 Thyroid Hormone Disorders and Sepsis – PubMed
“Clinical reports have shown that sepsis was often accompanied by thyroid dysfunction, which is called “low triiodothyronine (T3)” syndrome and characterized by decreased blood total T3 and free T3, and by normal or decreased thyroxine (T4) and thyroid stimulating hormone (TSH)”.
I suffer from Underactive Thyroid (Originally diagnosed with Graves Disease) when I was in the early stages of Sepsis, my thyroid became low, and my liver was also..
7. Periwound Skin Management
I have learned that my scar is an Atrophic Scar. I had a peri-wound – wound that is just above the bone
“The goal of peri-wound management is to maintain an optimal moist wound healing environment while preventing skin breakdown and infection. Skin is more vulnerable in patients with certain comorbidities and conditions. Periwound skin breakdown is just one of the culprits that delay wound healing and increase pain”. (28 Feb 2019).
7.2 How to Get Rid of Old Scars: Top 10 Remedies – Healthline
“Learn the top 10 home remedies for getting rid of old scars. Do you have a scar that makes you feel self-conscious? You’re not alone”.
8. Peeling Skin
8.1 Why does skin infection make skin peel?
“Certain types of staphylococci bacteria secrete toxic substances that cause the top layer of the skin (epidermis) to split from the rest of the skin. Because the toxin spreads throughout the body, staphylococcal infection of a small area of skin may result in peeling over the entire body”.
(I DID NOT LINK TO THIS ARTICLE AS IT HAS IMAGES)
8.2 Peeling Skin
“(21 Oct 2018) — What causes peeling skin? Many conditions, disorders or diseases can cause the skin to peel during the healing phase of the injury. Immediately”…
8.3 Skin Conditions: Understanding Your Skin – WebMD
“(26 Jul 2021) — Skin Conditions: Understanding Your Skin · Skin Layers · Epidermis: The Outer Layer of Skin · Dermis: The Middle Layer · Hypodermis: The Fatty Layer”.
9. Our Final Thoughts/Our YouTube Video
This topic took a bit of time to put together. I will admit I felt slightly anxious about doing this as a topic because to an extent it feels like ultimate exposure. BUT what made me puruse with it is, that if this is read by one person and it helps to give them a different perspective or might have some information that they previously might not have known, then this is more than worthit. Sharing our story in all its aspects is what we are doing, and this happened to be part of mine.
I hope this has been put together in a way that can make sense to those who read it. And as always we would like to wish you a safe day, evening and night.






7 thoughts on “My experience of: Pilonidal Cyst/Abscess Surgery: Staphylococcus Aureus bacteria/Sepsis (early stages)”